Sustainable employability in healthcare: a design problem
Every year, thousands of healthcare professionals leave the sector for good. The context structurally depletes their energy, even when the work itself still matters to them. The staffing shortage in healthcare is, at its core, a design problem rather than a recruitment challenge.
HR departments in healthcare know this, and they act on it. They launch vitality programmes, track absenteeism and send people to coaches. Turnover keeps rising anyway, burnout rates increase and waiting lists grow. The reason is simple: most interventions target the individual, while the problem lies in the context.
Sustainable employability in healthcare is, first and foremost, a behavioural challenge. Behavioural challenges are solved by redesigning the environment, rather than asking people to push harder.
Sustainable employability in healthcare is the capacity of healthcare professionals to remain healthy, motivated and productive now and in the future, in a sector with structurally high workload and emotional demands. It is a design challenge, and not so much an HR policy matter: context determines whether people can sustain their work, rather than individual motivation or willpower. More on Behavioural Design for HR →
Why the standard approach does not work
The classic approach to sustainable employability in healthcare revolves around three types of intervention: prevention (health checks, risk assessments, absenteeism tracking), treatment (coaching, career conversations, reintegration programmes) and awareness (campaigns about self-care, mindfulness, work-life balance).
All of these approaches share one assumption: the problem lies with the individual. When someone burns out, that person needs to change. Build more resilience. Take better care of themselves. Learn to set boundaries.
But behavioural science tells us something different. Most behavioural problems are context problems, not character flaws. When healthcare professionals structurally exhaust themselves, it is rarely because they lack resilience. It is almost always because the environment is designed in a way that makes exhaustion the logical outcome.[1]
Sustainable employability in healthcare is about raising the limit by redesigning the environment, and not so much about asking more of people who are already at theirs.
As long as administrative burden remains high, as long as healthcare professionals have little control over their own schedule and patient contact, as long as recovery is not structurally built in but depends on the goodwill of the team, nothing fundamentally changes. More training courses will not help.
Sustainable employability as a behavioural challenge
To design sustainable employability in healthcare, you first need to understand which forces drive healthcare professionals' behaviour. For that, we use the SUE Influence Framework, an analytical tool that maps the unconscious drivers behind behaviour.[2]
The Influence Framework asks five questions: What is the healthcare professional's Job-to-be-Done? What Pains do they experience in their current situation? What Gains would move them towards different behaviour? What Anxieties hold them back from changing? And what Comforts keep them stuck in existing patterns, even when those patterns are harmful?
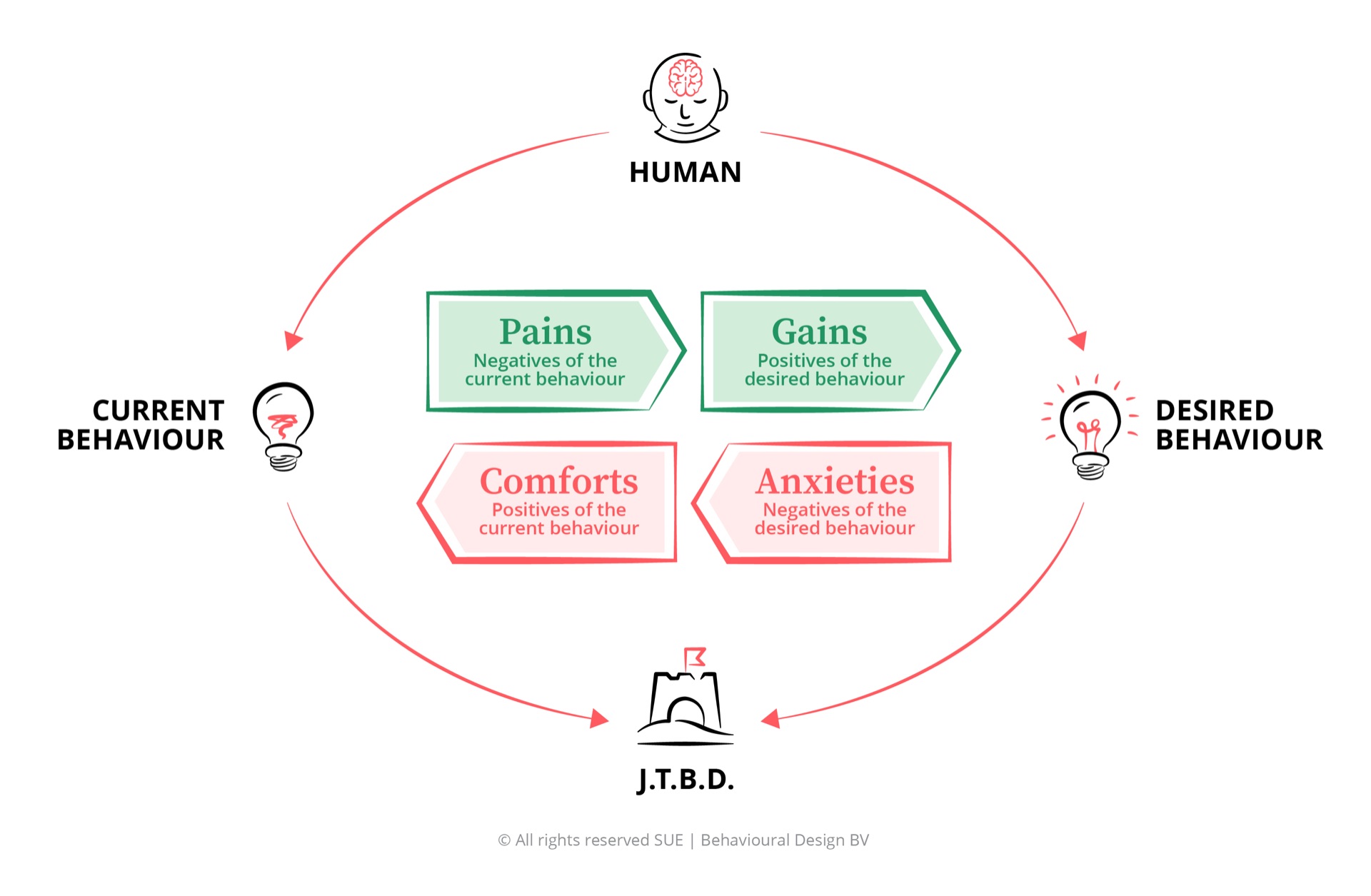
When you apply this framework to healthcare professionals, a recognisable pattern emerges:
Pains: The biggest pain is the loss of control, rather than the long working days themselves. Healthcare workers chose this profession from intrinsic motivation: helping people, making a difference, doing meaningful work. The pain lies in the sense that they can no longer deliver on that core purpose because too much time goes to administration, meetings and systems that do not work.
Comforts: The same strong intrinsic motivation is also the comfort that keeps people locked into exhausting patterns. Healthcare professionals do not quit, because they fundamentally believe the work matters. They keep going, even at the cost of their own health. The calling becomes a trap that delays breakdown without preventing it.
Anxieties: The threshold for asking for help or setting limits is enormous. There is fear of colleagues' judgement ("I am letting them down"), fear for professional identity ("I am not someone who cannot cope") and fear of consequences ("if I do less, who picks it up?"). These anxieties keep people moving even when stopping would be wiser.
Gains: The gains of well-designed sustainable employability are powerful: more time for patient contact, greater professional autonomy, the sense of being able to sustain the work without losing yourself. But they are abstract and distant, while today's pains are concrete and immediate.
How to design sustainable employability in healthcare
Once the Influence Framework analysis makes clear why healthcare professionals are stuck in exhausting patterns, the next question is: how do you design a context that changes this? For that, we use the SWAC model, which describes the four elements that together determine whether behaviour change succeeds: Spark, Want, Again and Can.[3]
The core insight of SWAC is that all four elements work multiplicatively. If one element is missing, the result is zero. This is why many HR programmes fail: they invest only in WANT (motivation, awareness, attitude change) while the real problem lies in CAN.
CAN: make the desired behaviour easy
The most powerful lever for sustainable employability in healthcare is lowering barriers to recovery and self-care. This means designing the environment so that the desired behaviour becomes the path of least resistance, rather than asking people to try harder.
In practice, this means: structurally reducing administrative burden through better systems or AI-supported documentation. Designing shift schedules that treat recovery time not as a luxury but as a design requirement. Fixed moments for team communication that are not cancelled when things get busy. Clear agreements about availability outside working hours.
Each of these changes makes the desired behaviour (stopping on time, recovering, setting limits) easier without requiring extra willpower from the individual. That is precisely the point. Behavioural design is not about demanding more from people. It is about designing the situation more intelligently.
SPARK: activate early, at the right moment
Many healthcare professionals only recognise the signs of exhaustion when they have already gone too far. The art is to build in spark moments that provide early signals, before it is too late. This can happen through team conversations that structurally make space for "how are you really doing?", through peer coaching where colleagues actively check in with each other, or through simple check-ins that become part of the regular team routine.
Importantly: the spark only works if something is done with it. A check-in without follow-up is a formality, not a spark. The moment of recognition must be linked to a clear next step.
WANT: restore intrinsic motivation
Healthcare professionals chose this work from a deep sense of purpose. Sustainable employability benefits from restoring that sense of purpose, not from adding more administrative obligations around vitality. This means giving people back professional autonomy. Let them influence their schedule, their patient mix, their career development. When the connection between the work and personal drive is restored, motivation rises organically.
AGAIN: make recovery a habit
One-off interventions do not work. Sustainable employability requires rhythm. That rhythm must be designed as a routine that does not depend on individual discipline. Think of fixed debriefs after intensive shifts, structured team conversations about workload as a standing agenda item, and peer support that is expected rather than voluntary.
The broader approach to sustainable employability through behavioural design describes how these principles apply across sectors. In healthcare the stakes are especially high, but the behavioural mechanisms are universal.
Concrete steps for HR in healthcare
How do you start with behavioural design for sustainable employability in healthcare? Begin with a thorough analysis of the behavioural forces in your organisation, rather than a new policy document. These are the first three steps:
1. Conduct six interviews with healthcare professionals at different levels. Do not ask what they think, ask what they do. What do they do when it gets too busy? When do they stop? When do they ask for help? Which moments are the hardest? The answers reveal the real comforts, anxieties and pains in the organisation.
2. Map the context, not the individuals. Look at rosters, systems, meeting structures and decision-making processes. Which elements of the work environment make it structurally harder for healthcare professionals to display the desired behaviour (recovering, setting limits, asking for help)?
3. Design one concrete CAN intervention as your starting point. Choose one barrier that you can remove or lower, and do it well. Simplicity and consistency are more powerful than a broad programme that inspires everyone but changes no one.
Frequently asked questions about sustainable employability in healthcare
What is sustainable employability in healthcare?
Sustainable employability in healthcare is the capacity of healthcare professionals to remain healthy, motivated and productive now and in the future. It goes beyond preventing absenteeism to designing a work context that structurally supports healthcare workers in their vitality, autonomy and sense of purpose.
Why is sustainable employability in healthcare so difficult to improve?
Most HR interventions target the individual: resilience training, mindfulness, wellness programmes. But the root cause lies in the context: structural administrative burden, lack of autonomy and insufficient recovery time. As long as the environment does not change, outcomes do not change.
How does Behavioural Design help with sustainable employability in healthcare?
Behavioural Design uses the SUE Influence Framework to map the forces driving healthcare professionals' behaviour: their motivations (pains and gains), what keeps them trapped in exhausting patterns (comforts) and the barriers to recovery (anxieties). From those insights you design interventions that change the context, not the individual.
What are concrete interventions for sustainable employability in healthcare?
Concrete interventions include: radically reducing administrative burden through better systems or AI-supported documentation (CAN), redesigning shift schedules so that recovery is a structural requirement rather than a luxury (AGAIN), restoring professional autonomy (WANT) and building in early warning moments for exhaustion (SPARK). The key is system design, not individual behavioural coaching.

1.5 minutes of Influence
Read by 10,000+ professionals · Free · Unsubscribe any time


